


Non-compaction cardiomyopathy (NCCM) is a rare but significant heart condition that brings unique challenges for diagnosis and management. As the heart muscle fails to compact properly during fetal development, it can lead to serious complications, including heart failure and arrhythmias. This is especially concerning for older adults, whose symptoms may often be overlooked.
In this article, we’ll explore the intricacies of NCCM, focusing on essential diagnostic criteria, innovative treatment options, and promising avenues for future research. How can healthcare professionals enhance their understanding and management of this complex condition to improve patient outcomes?
By addressing these questions, we aim to foster a deeper understanding of NCCM and encourage proactive care. Together, we can work towards better health outcomes for those affected by this condition.
is a rare and complex condition that impacts the structure of the heart muscle, especially the left ventricle. This condition occurs when the heart muscle doesn’t compact properly during fetal development, leading to a spongy appearance with prominent trabeculations and deep intertrabecular recesses. Unfortunately, it can lead to , such as , arrhythmias, and thromboembolic events, with about two-thirds of individuals experiencing heart failure over time.
For elderly patients, the impact of non-communicable chronic diseases can be especially pronounced. They may present with . For instance, consider an 85-year-old woman who had a left ventricular ejection fraction (LVEF) of 25-30%. She was diagnosed with non-compaction cardiomyopathy after she experienced chest pain and dyspnea. This case underscores the importance of heightened awareness among healthcare providers. Misdiagnosis is common in older adults due to overlapping health issues, making for effective management.
Recent studies have shown that incorporating family and genetic information can significantly aid in diagnosing this condition, as familial recurrence is more common in adults than in children. The establishment of echocardiographic diagnostic criteria has improved recognition rates, leading to better outcomes for individuals. For example, a study involving 34 adults with isolated non-communicable chronic muscle disease revealed a 58% probability of event-free survival at five years, highlighting the serious implications of this condition.
Healthcare specialists emphasize the importance of for individuals diagnosed with non-compaction cardiomyopathy, particularly those at risk of cardiac arrest. Procedures like implantable cardioverter defibrillators (ICDs) may be recommended for individuals with significant arrhythmias. As one cardiologist noted, 'Increased awareness of non-compaction cardiomyopathy and the use of are vital for enhancing recognition and handling in older adults.' This statement reflects the critical role of ongoing education and research in improving the quality of care for those affected by non-compaction cardiomyopathy.
At Amavita, our exemplifies our commitment to providing comprehensive cardiovascular management. We integrate and personalized treatment plans to improve outcomes for patients with non-compaction cardiomyopathy. If you or a loved one are facing challenges related to this condition, please reach out. We’re here to support you every step of the way.

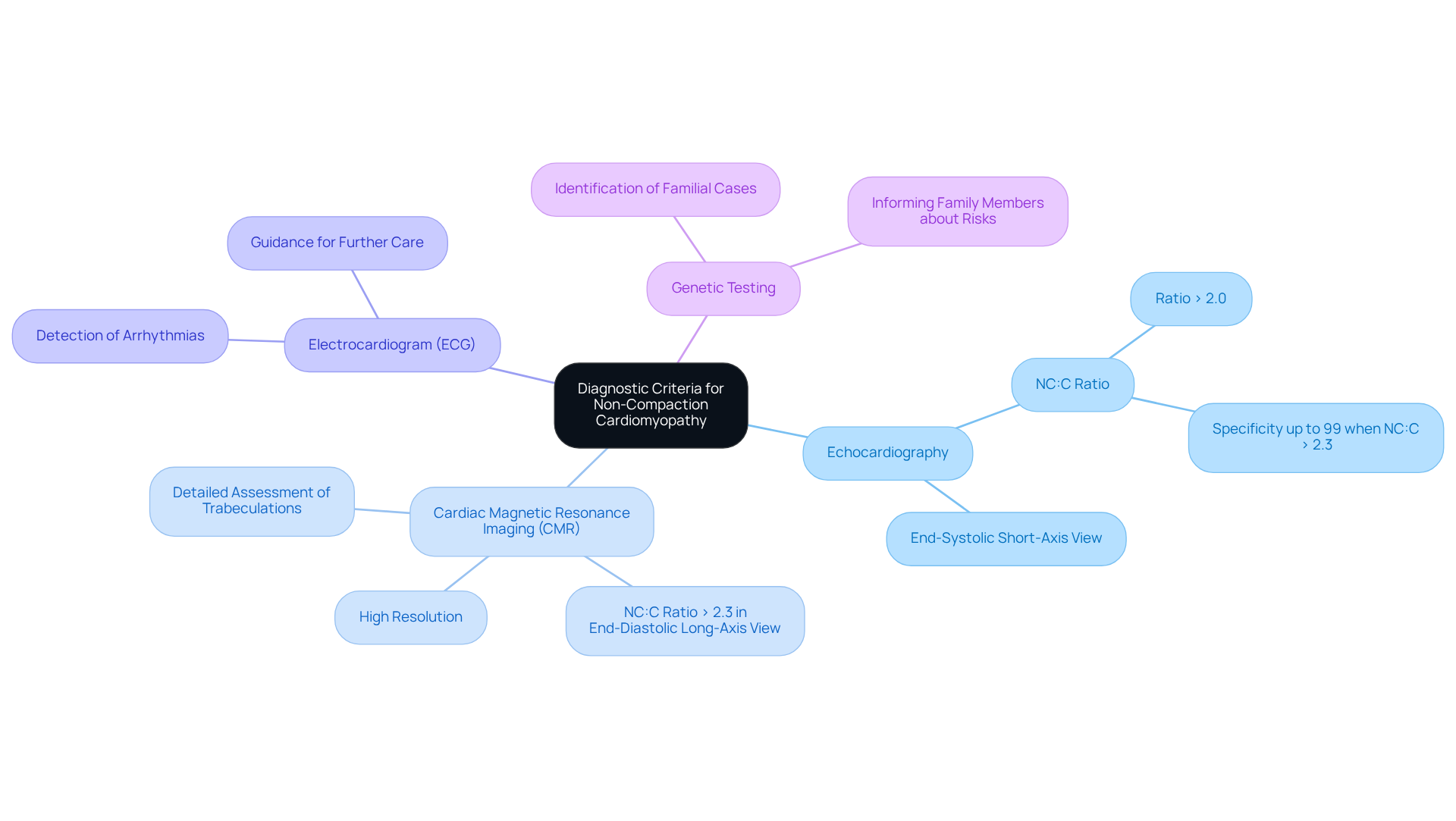
Diagnosing is a journey that necessitates a thoughtful and comprehensive approach, integrating clinical evaluation with available at Amavita Heart and Vascular Health. It’s important to understand the key diagnostic criteria that can help in this process:
Utilizing these diagnostic tools effectively at Amavita is crucial for early detection and better management strategies for individuals experiencing non-cardiac chest pain. By focusing on early intervention, we aim to improve outcomes and reduce hospital readmissions, ensuring that you feel supported every step of the way.
Managing non-compaction cardiomyopathy (NCCM) focuses on you-your symptoms, your health, and your needs. Let’s explore some that can make a difference:
By embracing a comprehensive management strategy that includes these elements, you can greatly enhance your . Remember, you’re not alone in this journey-support is always available to ensure you receive the best care tailored just for you.

Future research in non-compaction cardiomyopathy focuses on several key areas that hold promise for improving patient care and treatment outcomes.
By focusing on these innovative research directions, the medical community aims to deepen the understanding and management of non-compaction cardiomyopathy. This commitment ultimately seeks to improve patient outcomes and enhance quality of life, reassuring patients that they are not alone in their journey.

Non-compaction cardiomyopathy (NCCM) is a complex and often underrecognized condition that can deeply impact heart structure and function, especially in the left ventricle. This condition arises from improper compaction during fetal development, leading to serious complications. It’s essential for healthcare professionals to increase their awareness and understanding of NCCM, as this can significantly affect patient outcomes.
The article sheds light on several critical aspects of NCCM. Diagnosis often relies on advanced imaging techniques like echocardiography and cardiac magnetic resonance imaging. Additionally, genetic testing plays a vital role in familial cases. Treatment strategies vary, encompassing medications, device therapy, and lifestyle changes, all aimed at enhancing the quality of life for patients and preventing severe outcomes such as heart failure and arrhythmias. Ongoing research into genetic factors and innovative therapies offers hope for better management and outcomes for those affected by this rare condition.
As the medical community continues to deepen its understanding of non-compaction cardiomyopathy, it’s crucial for both patients and healthcare providers to stay informed about the latest diagnostic and treatment options. By fostering a proactive approach to care and supporting ongoing research efforts, we can look forward to improved management strategies that significantly enhance the lives of individuals living with NCCM. Awareness and education are key to ensuring timely diagnosis and effective interventions, ultimately leading to better outcomes for patients facing this challenging condition.
Have you or a loved one been affected by NCCM? Remember, you’re not alone in this journey. Reach out for support, and let’s work together towards a brighter future.
What is non-compaction cardiomyopathy?
Non-compaction cardiomyopathy is a rare condition that affects the structure of the heart muscle, particularly the left ventricle, resulting in a spongy appearance due to improper compaction during fetal development.
What are the potential complications of non-compaction cardiomyopathy?
Complications can include heart failure, arrhythmias, and thromboembolic events, with approximately two-thirds of individuals experiencing heart failure over time.
Why is early diagnosis important for non-compaction cardiomyopathy, especially in elderly patients?
Early diagnosis is crucial because elderly patients may present with atypical symptoms that complicate diagnosis, leading to potential misdiagnosis. Recognizing the condition early can improve management and outcomes.
How can family and genetic information assist in diagnosing non-compaction cardiomyopathy?
Incorporating family and genetic information can aid in diagnosis since familial recurrence is more common in adults than in children, helping healthcare providers identify the condition more effectively.
What advancements have been made in the diagnosis of non-compaction cardiomyopathy?
The establishment of echocardiographic diagnostic criteria has improved recognition rates of the condition, leading to better outcomes for individuals diagnosed with it.
What is the significance of follow-ups for patients with non-compaction cardiomyopathy?
Consistent follow-ups and supervision are vital for individuals diagnosed with non-compaction cardiomyopathy, especially those at risk of cardiac arrest, to ensure proper management and care.
What treatments may be recommended for individuals with significant arrhythmias due to non-compaction cardiomyopathy?
Procedures such as implantable cardioverter defibrillators (ICDs) may be recommended for individuals experiencing significant arrhythmias.
How does the CardioElite™ program at Amavita support patients with non-compaction cardiomyopathy?
The CardioElite™ program provides comprehensive cardiovascular management through advanced diagnostic tools and personalized treatment plans to improve outcomes for patients facing challenges related to non-compaction cardiomyopathy.