


Heart failure is a pressing health issue that affects millions, yet many remain unaware of its complexities and implications. This condition, characterized by the heart's inability to pump blood effectively, can stem from various causes, including valve disease and underlying health issues such as hypertension and diabetes. As the number of individuals diagnosed with heart failure continues to rise, understanding its symptoms, risk factors, and treatment options becomes crucial. How can patients and caregivers navigate this intricate landscape to ensure timely intervention and effective management of heart health?
In addition to this, recognizing the signs of heart failure is essential. Symptoms may include:
By being aware of these indicators, patients can take proactive steps toward seeking medical advice. Furthermore, managing risk factors—such as maintaining a healthy diet, exercising regularly, and adhering to prescribed medications—plays a significant role in heart health.
Ultimately, it is important to remember that support is available. Patients and caregivers are encouraged to reach out to healthcare professionals for guidance and assistance. Together, we can navigate the complexities of heart failure and work towards a healthier future.
can feel overwhelming, as it represents a complex clinical syndrome where the to meet the body's needs. This condition may stem from various underlying issues, such as weakened cardiac muscles or stiffening of the heart walls. One significant contributor to cardiac problems is , which occurs when valves do not open or close properly, forcing the heart to work harder. This added strain can lead to symptoms like breathlessness and fatigue, particularly during everyday activities.
It's essential to recognize that cardiac insufficiency is not merely one condition; rather, it encompasses a range of symptoms arising from different cardiovascular challenges. Understanding involves recognizing its forms, including heart failure with reduced ejection fraction (HFrEF) and preserved ejection fraction (HFpEF). Each type presents unique challenges and treatment options. Recent studies reveal that more than half of the approximately 6.7 million Americans living with cardiac dysfunction have , a condition increasingly prevalent among older adults and those facing additional health concerns such as hypertension and obesity.
At Amavita Cardiac and Vascular Health, we are dedicated to providing to uncover the specific causes behind fatigue and breathlessness. This allows us to create aimed at and restoring energy levels. Addressing valve disease is vital, as neglecting these issues can lead to serious consequences, including cardiac collapse. With projections indicating that the number of individuals with cardiac problems may rise to 8.7 million by 2030, understanding these distinctions is crucial for both patients and caregivers. It empowers them to navigate the complexities of cardiovascular health and treatment options with confidence.
Moreover, it's important to acknowledge that the , underscoring the need for targeted public health strategies to address these disparities. The lifetime risk of developing heart failure is estimated at 24%, highlighting the urgent public health challenge posed by this condition. Together, we can raise awareness and implement intervention strategies that truly make a difference in the lives of those affected.

Cardiac dysfunction can arise from various factors, including , hypertension, diabetes, and valvular cardiac disease, potentially leading to . It's important to recognize that —like smoking and physical inactivity—play a significant role. For older individuals, the combined impact of these elements can lead to a higher occurrence of cardiac issues. Therefore, it is essential for everyone, especially seniors, to be mindful of these factors and participate in to keep track of their cardiovascular health.
Recent studies reveal that , a number that is anticipated to rise to 11.4 million by 2050. Alarmingly, one in four Americans will face heart failure during their lifetime, highlighting the widespread nature of this concern. By understanding these causes and risk factors of heart failure, patients can collaborate with healthcare providers to create that suit their unique needs.
In addition to this, innovative , such as the portable, FDA-cleared AI ultrasound utilized at Amavita Heart and Vascular Health®, is making strides in early detection and informed decision-making. This technology not only provides real-time guidance for precise imaging but also generates reports on cardiac structure and function within minutes, significantly and potentially reducing hospital readmissions.
Furthermore, addressing is vital for effective management of heart failure, as these challenges can greatly impact treatment outcomes. Remember, you are not alone in this journey; , and taking proactive steps toward your heart health can lead to a brighter, healthier future.

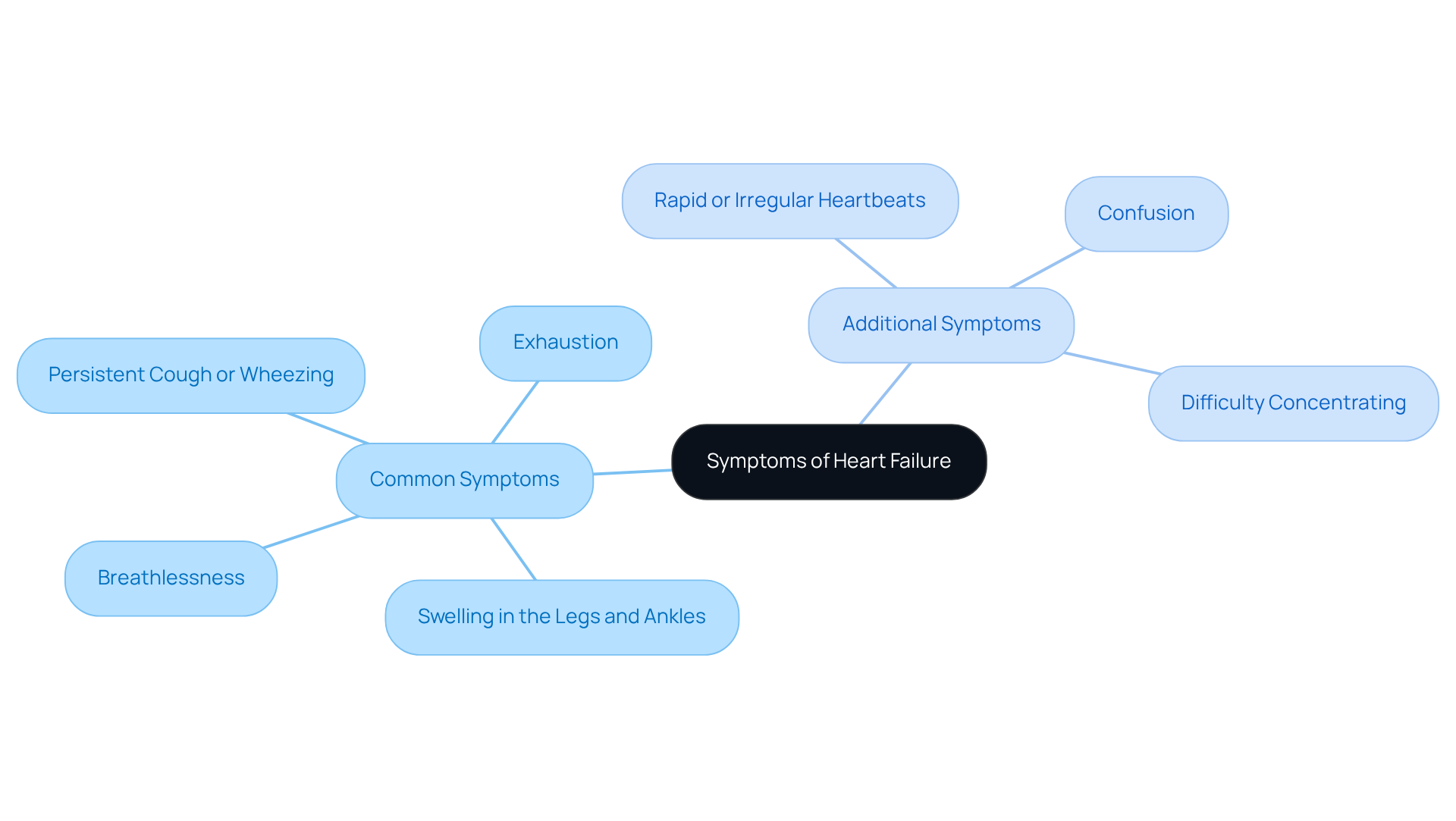
Are you or a loved one experiencing signs of ? Common symptoms of include:
It's important to be aware that patients may also face:
These can be symptoms of heart failure. For older individuals, these signs can sometimes be mistaken for typical aging, making it essential for caregivers and family members to stay vigilant. can be lifesaving, as heart failure often requires immediate care.
Research shows that individuals with cardiac problems have about a 50 percent chance of surviving five years after their first hospitalization. Alarmingly, the number of people facing cardiac issues is projected to rise to 8.7 million by 2030. This underscores the and prompt identification of symptoms. , leading to feelings of sadness or depression.
Healthcare professionals emphasize the importance of recognizing potential triggers, as Dr. Pelter notes, because early detection can lead to of heart failure. At Amavita Heart and Vascular Health, we are dedicated to providing specialized for high-risk patients. Our approach includes advanced imaging and comprehensive evaluations to ensure that any issues are accurately assessed and managed.
Understanding how cardiovascular issues present differently in older adults is crucial for . These individuals may show atypical signs that require careful observation and evaluation. Remember, you are not alone in this journey, and we are here to support you every step of the way.
Understanding cardiac dysfunction can feel overwhelming, but it is essential to approach it with a that includes your medical history, physical assessment, and a variety of . Key tests, such as blood examinations, help assess specific indicators like B-type natriuretic peptide (BNP), which is crucial for confirming cardiac dysfunction. Chest X-rays allow us to evaluate cardiac size and check for fluid accumulation in the lungs, while are vital for assessing cardiac function and structure. These imaging studies can reveal irregularities in cardiac motion and valve function, making them indispensable in diagnosing cardiac issues.
Recent advancements in echocardiography have made it even more effective, enabling precise evaluations of cardiac conditions. For instance, studies show that echocardiograms can identify heart failure, specifically , which affects over half of the heart failure population and carries a one-year mortality rate of 20-29%. Furthermore, the integration of is improving diagnostic accuracy, allowing for earlier detection of individuals at high risk. As specialists have noted, "AI is assisting clinicians in recognizing high-risk individuals sooner, allowing intervention before disease advances."
In addition to echocardiograms, electrocardiograms (EKGs) and stress tests are commonly used to assess cardiac rhythm and function under physical stress. may also be performed to visualize coronary arteries and check for blockages, especially in those with suspected coronary artery disease.
Real-world examples underscore the significance of these diagnostic methods. For example, a research project examining the risk of cardiovascular complications linked to various treatments found that proper diagnosis and management can significantly influence individual outcomes. Additionally, the American College of Cardiology emphasizes the need for guideline-directed medical therapy once heart failure is identified, highlighting the crucial role of for individuals.
By understanding these diagnostic tests and their implications, you can feel more empowered and engaged in your healthcare journey, fostering a collaborative relationship with your healthcare providers. Programs like , described as a 'clinical force multiplier,' enhance this process by offering advanced, real-time diagnostic data and . This integration ultimately transforms cardiac care and reduces readmissions in skilled nursing facilities, ensuring that elderly individuals receive thorough and proactive management of their cardiovascular health.

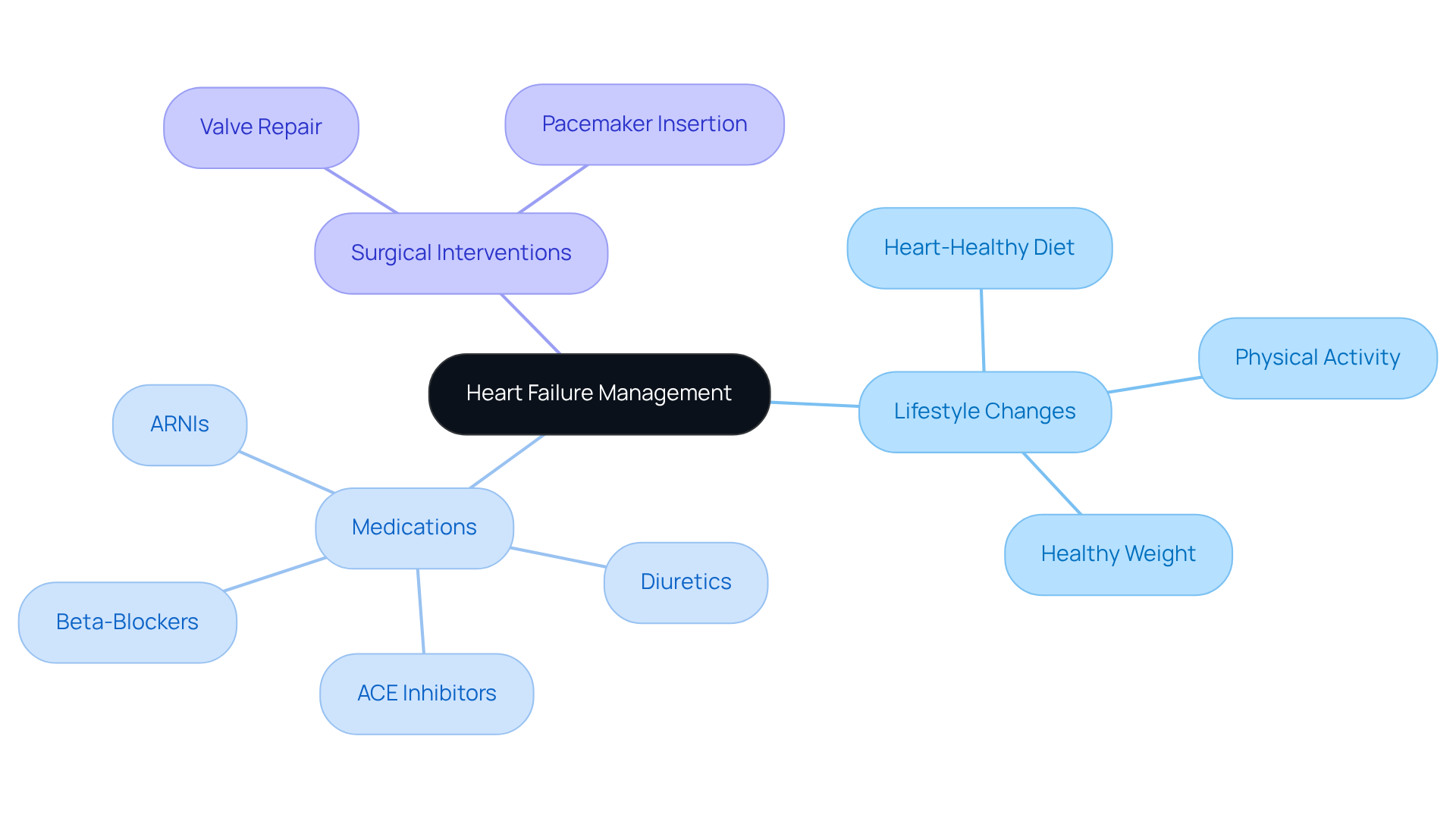
Effectively managing is a journey that involves a blend of , medications, and sometimes, . For elderly patients, foundational lifestyle modifications are essential. Consider adopting a , engaging in , and maintaining a healthy weight. These changes not only help alleviate symptoms but also enhance your overall well-being.
Medications are a vital part of your treatment plan. Options like diuretics, ACE inhibitors, beta-blockers, and newer agents such as angiotensin receptor-neprilysin inhibitors (ARNIs) are commonly prescribed. These medications work to and lower the risk of hospitalization, offering you a chance to avoid heart failure and achieve a healthier heart.
In , surgical interventions may be necessary. Methods such as valve repair or the insertion of devices like pacemakers can provide substantial benefits. Many individuals who embrace lifestyle changes alongside medical treatment often report an and fewer symptoms.
Real-world examples illustrate the effectiveness of these lifestyle modifications. Numerous individuals have successfully managed their cardiac issues by incorporating consistent workout practices and dietary changes, leading to . By understanding and implementing these treatment options, you can actively participate in your care, ultimately working towards better heart health and reducing the risk of heart failure for a more fulfilling quality of life. Remember, you are not alone on this journey; support is always available to help you every step of the way.
Understanding heart failure is vital for navigating the complexities of cardiovascular health. This multifaceted condition not only affects the heart's ability to pump blood effectively but also includes a variety of causes, symptoms, and treatment options. By grasping the fundamental aspects of heart failure, individuals can better advocate for their health and engage in proactive management strategies.
The article explores the various causes and risk factors associated with heart failure, such as:
Recognizing symptoms early is crucial, as timely intervention can significantly improve outcomes. Diagnostic procedures, including:
play a pivotal role in identifying heart failure. Moreover, a combination of lifestyle changes, medications, and surgical options offers pathways to effective management.
Ultimately, raising awareness about heart failure is essential for both individuals and communities. With the projected rise in cases, especially among vulnerable populations, it is imperative to prioritize heart health through:
By taking informed steps and collaborating with healthcare providers, individuals can navigate their journey toward better heart health. This proactive approach can make a meaningful impact on their quality of life and help alleviate the burden of this condition on society.
What is heart failure?
Heart failure is a complex clinical syndrome where the heart struggles to pump blood effectively to meet the body's needs. It can arise from various underlying issues, such as weakened cardiac muscles or stiffening of the heart walls.
What are the main types of heart failure?
The main types of heart failure are heart failure with reduced ejection fraction (HFrEF) and heart failure with preserved ejection fraction (HFpEF). Each type presents unique challenges and treatment options.
What are the common symptoms of heart failure?
Common symptoms of heart failure include breathlessness and fatigue, particularly during everyday activities.
What are the primary causes of heart failure?
Primary causes of heart failure include coronary artery disease, hypertension, diabetes, and valvular cardiac disease.
What risk factors contribute to heart failure?
Risk factors for heart failure include age, family history, obesity, smoking, physical inactivity, and other lifestyle choices.
How prevalent is heart failure in the United States?
Approximately 6.7 million Americans over the age of 20 are living with heart failure, and this number is expected to rise to 11.4 million by 2050. One in four Americans will face heart failure during their lifetime.
How can individuals manage their risk for heart failure?
Individuals can manage their risk for heart failure by understanding their causes and risk factors, participating in regular health screenings, and collaborating with healthcare providers to create personalized prevention strategies.
What role does technology play in heart failure detection?
Innovative AI-powered diagnostic technology, such as portable, FDA-cleared AI ultrasound, enhances early detection and informed decision-making by providing real-time guidance for precise imaging and generating reports on cardiac structure and function quickly.
Why is it important to address healthcare access in heart failure management?
Addressing systemic barriers to healthcare access is crucial for effective management of heart failure, as these challenges can significantly impact treatment outcomes.
What is the lifetime risk of developing heart failure?
The lifetime risk of developing heart failure is estimated at 24%.